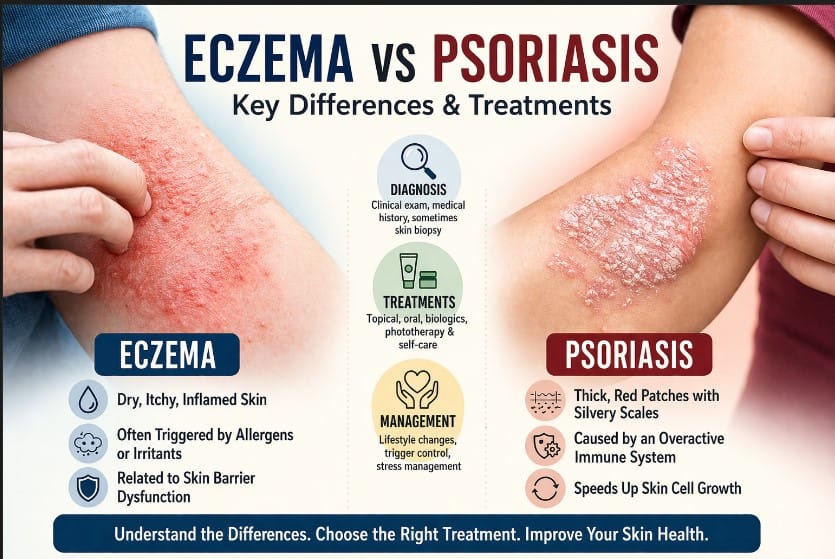
Eczema vs Psoriasis: Key Differences and Treatments
Understanding the difference between Eczema and Psoriasis is essential because although both affect the skin and can look similar at times, they are fundamentally different in their causes, symptoms, and treatments. Misidentification can lead to ineffective treatment and prolonged discomfort.
This guide explains both conditions in detail, starting with their definitions, causes, symptoms, and how to distinguish between them.
What is Eczema?
Eczema (also known as atopic dermatitis) is a chronic inflammatory skin condition that causes dry, itchy, and inflamed skin. It often begins in childhood but can appear at any age.
Eczema is not contagious, but it tends to run in families with a history of allergies, asthma, or hay fever.
Common Characteristics of Eczema:
- Dry, sensitive skin
- Intense itching (often worse at night)
- Red or inflamed patches
- Cracked or rough skin
- Oozing or crusting in severe cases
Eczema tends to come and go in flare-ups, meaning symptoms can worsen at certain times and improve at others.
What is Psoriasis?
Psoriasis is a chronic autoimmune condition that speeds up the life cycle of skin cells. This leads to a buildup of cells on the skin surface, forming thick, scaly patches.
Unlike eczema, psoriasis is primarily driven by an overactive immune system rather than external irritants or allergens.
Common Characteristics of Psoriasis:
- Thick, raised patches of skin
- Silvery-white scales
- Dry, cracked skin that may bleed
- Itching or burning sensation
- Patches often appear symmetrical
Psoriasis is also a long-term condition with periods of flare-ups and remission.
Causes: How They Differ
Although both conditions involve inflammation, their root causes are different.
Causes of Eczema:
Eczema is linked to a combination of genetic and environmental factors, including:
- Overactive immune response to irritants
- Skin barrier dysfunction (leads to moisture loss)
- Allergens such as dust, pollen, or certain foods
- Harsh soaps or chemicals
- Weather changes (cold, dry air)
People with eczema often have a weakened skin barrier, making their skin more prone to dryness and irritation.
Causes of Psoriasis:
Psoriasis is an autoimmune disorder where the immune system mistakenly attacks healthy skin cells.
Key factors include:
- Immune system dysfunction
- Genetic predisposition
- Triggers such as stress, infections, or injuries
- Certain medications
- Lifestyle factors like smoking or alcohol consumption
In psoriasis, the skin cells multiply much faster than normal, leading to visible plaques.
Symptoms Comparison
Although both conditions cause skin inflammation, their symptoms differ in appearance and sensation.
Eczema Symptoms:
- Severe itching (primary symptom)
- Dry, flaky skin
- Red or brownish patches
- Common in areas like elbows, behind knees, neck, and face
- Skin may ooze or become crusty during flare-ups
Psoriasis Symptoms:
- Thick, scaly plaques with clear borders
- Silvery-white scales
- Common on elbows, knees, scalp, and lower back
- Itching may be mild to moderate
- Skin may crack and bleed in severe cases
Appearance Differences
One of the easiest ways to distinguish between eczema and psoriasis is by observing the skin’s appearance.
- Eczema patches are usually softer, less defined, and more inflamed, often appearing red or brown depending on skin tone.
- Psoriasis patches are thicker, well-defined, and covered with silvery scales.
Common Areas Affected
Both conditions can appear anywhere on the body, but they tend to favor certain regions.
Eczema:
- Inner elbows
- Behind knees
- Face and neck
- Hands and wrists
- Ankles
Psoriasis:
- Elbows
- Knees
- Scalp
- Lower back
- Nails (nail pitting or discoloration)
Age and Onset
- Eczema commonly begins in infancy or early childhood, although adults can also develop it later in life.
- Psoriasis typically develops between ages 15 and 35, though it can occur at any age.
Triggers and Flare-ups
Both conditions are chronic, but flare-ups are triggered by different factors.
Eczema Triggers:
- Allergens (dust mites, pollen)
- Irritants (soaps, detergents, fragrances)
- Weather (cold, dry air)
- Stress
- Sweating
Psoriasis Triggers:
- Stress
- Infections (such as strep throat)
- Skin injuries (cuts, sunburns)
- Certain medications
- Smoking and alcohol
Underlying Mechanism
Understanding how each condition affects the body helps clarify why treatments differ.
Eczema Mechanism:
Eczema involves a weakened skin barrier that allows moisture to escape and irritants to enter. This triggers inflammation and itching.
Psoriasis Mechanism:
Psoriasis is caused by an overactive immune system that accelerates skin cell turnover. Instead of shedding normally, skin cells accumulate on the surface.
Emotional and Lifestyle Impact
Both eczema and psoriasis can significantly affect quality of life.
- Chronic itching can disrupt sleep (more common in eczema).
- Visible skin lesions can impact self-esteem and confidence.
- Social anxiety and stress may worsen symptoms.
Managing these conditions often requires both physical treatment and emotional support.
Diagnosis
Doctors typically diagnose eczema or psoriasis through:
- Physical examination of the skin
- Medical history review
- Family history of allergies or autoimmune diseases
- In some cases, a skin biopsy to confirm the diagnosis
Accurate diagnosis is important because treatments for eczema and psoriasis differ significantly.
Treatment of Eczema
Treatment for Eczema mainly focuses on restoring the skin barrier, reducing inflammation, and relieving itching. Therefore, most treatment plans include a combination of topical care, medications, and lifestyle adjustments.
Topical Treatments
First and foremost, moisturizers play a key role. Regular use of fragrance-free emollients helps keep the skin hydrated and prevents dryness. As a result, flare-ups can be reduced.
In addition, doctors often prescribe topical corticosteroids. These medications help control inflammation and itching during flare-ups. Depending on the severity, mild to strong formulations may be used.
Furthermore, topical calcineurin inhibitors such as tacrolimus are sometimes recommended. These are especially useful for sensitive areas like the face and neck because they do not thin the skin like steroids.
Oral and Systemic Medications
When symptoms are moderate to severe, oral medications may be required. For instance, antihistamines are commonly used to reduce itching, particularly at night, which helps improve sleep.
In more persistent cases, oral corticosteroids may be prescribed for short-term relief. However, they are not suitable for long-term use due to side effects.
Additionally, immunosuppressant drugs may be used in chronic cases. These medications work by calming the immune response, thereby reducing inflammation.
Biologic Therapies
In recent years, biologic treatments have become an option for moderate to severe Eczema. These therapies target specific parts of the immune system. Consequently, they help control inflammation more precisely and effectively in patients who do not respond to conventional treatments.
Treatment of Psoriasis
Treatment for Psoriasis focuses on slowing down rapid skin cell production and controlling the immune system. Because psoriasis is an autoimmune condition, treatment approaches are often more long-term and systemic.
Topical Treatments
Initially, mild cases are treated with topical medications. For example, corticosteroid creams reduce redness, itching, and inflammation.
Similarly, vitamin D analogues are widely used. These help slow down the excessive growth of skin cells.
In addition, coal tar preparations can reduce scaling and itching. Although older, they are still effective for some patients.
Topical retinoids may also be prescribed. These help normalize skin cell turnover, thereby improving skin texture over time.
Phototherapy
When topical treatments are not sufficient, phototherapy is often recommended. This involves exposing the skin to controlled ultraviolet (UV) light under medical supervision.
As a result, skin cell growth slows down, and symptoms improve. Phototherapy is commonly used for moderate cases of Psoriasis.
Systemic Treatments
For more severe cases, systemic treatments may be necessary. These include oral medications such as methotrexate or cyclosporine. These drugs suppress the immune system and reduce inflammation throughout the body.
In addition, biologic therapies are widely used today. These medications target specific immune pathways, and therefore, they can provide long-term control with fewer side effects compared to traditional systemic drugs.
Natural and Home Care Approaches
Although medical treatment is essential, supportive home care can make a significant difference in managing both Eczema and Psoriasis.
For Eczema
To begin with, maintaining proper skin hydration is crucial. Frequent moisturizing helps prevent dryness and itching. Moreover, using mild, fragrance-free cleansers reduces irritation.
It is also important to avoid hot showers. Instead, lukewarm water is recommended because it does not strip the skin of natural oils.
Additionally, wearing soft, breathable fabrics like cotton can prevent skin irritation. At the same time, identifying and avoiding allergens such as dust mites, pollen, or certain foods can help reduce flare-ups.
For Psoriasis
Similarly, hydration is important for psoriasis as well. Keeping the skin moisturized helps reduce scaling and cracking.
Furthermore, medicated shampoos can be helpful for scalp psoriasis. These shampoos often contain ingredients that reduce scaling and inflammation.
In addition, it is advisable to avoid scratching plaques. Doing so can worsen the condition and may even lead to infection.
Equally important is stress management. Relaxation techniques such as meditation and breathing exercises can help reduce flare-ups.
Lifestyle Modifications
Lifestyle choices play a major role in controlling both conditions. Therefore, making healthy changes can significantly improve outcomes.
Stress Management
Stress is a well-known trigger for both Eczema and Psoriasis. Consequently, managing stress is essential. Practices such as yoga, meditation, and regular physical activity can help maintain emotional balance.
Diet and Nutrition
Although diet alone cannot cure these conditions, it can influence symptoms. For example, an anti-inflammatory diet rich in fruits, vegetables, nuts, and healthy fats may help reduce inflammation.
In some cases of eczema, certain foods may trigger reactions. Therefore, identifying and avoiding such foods can be beneficial.
Similarly, for psoriasis, maintaining a healthy weight and balanced diet supports overall immune health.
Sleep and Rest
Proper sleep is equally important. Poor sleep can worsen itching in Eczema and increase stress levels. As a result, maintaining a consistent sleep routine can help manage symptoms more effectively.
Preventing Flare-Ups
Although neither condition can be completely cured, flare-ups can be reduced with proper care.
For eczema, it is important to avoid harsh soaps, maintain skin hydration, and minimize exposure to known irritants. In contrast, for psoriasis, avoiding skin injuries, infections, smoking, and excessive alcohol consumption is recommended.
Moreover, following prescribed treatment plans consistently is crucial in both conditions. Skipping treatment often leads to recurrence or worsening of symptoms.
Possible Complications
If not managed properly, both conditions may lead to complications.
In eczema, frequent scratching can cause skin infections, thickened skin, and sleep disturbances. Over time, this may also affect emotional well-being.
On the other hand, psoriasis may lead to more serious complications such as psoriatic arthritis, which affects the joints. Additionally, long-term inflammation may increase the risk of cardiovascular problems.
When to Seek Medical Help
It is advisable to consult a doctor if symptoms become severe or do not improve with basic care. Similarly, medical attention is needed if the skin shows signs of infection such as pain, swelling, or pus.
Furthermore, if itching interferes with sleep or daily activities, professional evaluation is important. Early diagnosis and proper treatment can significantly improve the quality of life for individuals with Eczema or Psoriasis.
Final Thoughts
In conclusion, both Eczema and Psoriasis are chronic conditions that require long-term management. Although they share some similarities, their causes, symptoms, and treatments differ significantly.
Therefore, understanding these differences helps in choosing the right approach to care. With proper medical guidance, consistent skincare, and healthy lifestyle habits, it is possible to manage symptoms effectively and maintain healthy skin over time.
FAQs:
The main difference is the cause. Eczema is mainly related to skin barrier dysfunction and allergens, whereas psoriasis is an autoimmune condition caused by an overactive immune system.
No, eczema does not turn into psoriasis. They are two separate conditions with different underlying mechanisms. However, in rare cases, a person may develop both independently.
Eczema typically causes more intense itching compared to psoriasis. In eczema, itching is often severe and may worsen at night, while psoriasis usually causes mild to moderate itching.
Eczema flare-ups are commonly triggered by allergens, irritants, weather changes, and stress. Psoriasis flare-ups, on the other hand, are often triggered by stress, infections, skin injuries, certain medications, and lifestyle factors.
Yes, diet can play a supportive role. A balanced, anti-inflammatory diet may help reduce inflammation in both conditions. However, diet alone cannot cure either Eczema or Psoriasis.
Treatment usually includes moisturizers, topical corticosteroids, antihistamines, and in some cases, immunosuppressants or biologics. The choice depends on severity and individual response.